Partecipazione al Webinar di IEMIG – il 17 Giugno 2024 ore 18.00. Il webinar si terrà tramite piattaforma online. entrando in ZOOM al seguente link: Entra Zoom Riunione:https://us04web.zoom.us/j/4558342396?pwd=QkZyzXYGibx21pHzt5fPvRLu2o4dbu.1&omn=71242358198 ID riunione:

PREMIO DI STUDIO “VALENTINA LIBONI 2024”PREMIO DI STUDIO “VALENTINA LIBONI 2024”
PER LAUREATI NEL CORSO DI LAUREA IN MEDICINA E CHIRURGIA, CORSO DI LAUREA IN INFERMIERISTICA, E NEOSPECIALISTI DELLA SCUOLA DI SPECIALIZZAZIONE IN MEDICINA DI EMERGENZA-URGENZA Si rende noto che l’Associazione

I.E.M.I.G. – grati per il vostro impegno nel sostenere la nostra missione.I.E.M.I.G. – grati per il vostro impegno nel sostenere la nostra missione.
L’Associazione I.E.M.I.G. desidera esprimere la propria gratitudine alle seguenti aziende per il loro sostegno, l’evento è stato un grande successo e ha avuto un impatto positivo.“Benassi Assicurazioni, Costruzioni Nigro, Forseco

Buone Feste da I.E.M.I.G.Buone Feste da I.E.M.I.G.
La Direzione, Il Comitato Scientifico e tutta la Componente Organizzativa augura Buon Natale a tutti i Soci e Sostenitori.

La medicina d’urgenza conquista i giovani: tre borse di studio di IemigLa medicina d’urgenza conquista i giovani: tre borse di studio di Iemig
Fonte: Quotidiano La Nazione Cronaca di Prato del 20 Dicembre 2023 (Sa.Be) PRATO Il premio Valentina Liboni, giunto alla terza edizione e dedicato alla memoria dell’infermiera del pronto soccorso del

Premio Valentina Liboni 2023 a due medici e un’infermiera.Premio Valentina Liboni 2023 a due medici e un’infermiera.
Fonte: Notizie di prato (e.b) – Ieri sera all’Art hotel la consegna dei tre riconoscimenti ai giovani professionisti. Solo uno di loro lavora a Prato. La Medicina d’emergenza continua a

Vincitori del Premio “Valentina Liboni 2023”Vincitori del Premio “Valentina Liboni 2023”
Siamo lieti di annunciare i tre vincitori del prestigioso “Premio Valentina Liboni 2023”. Questo premio celebra le migliori Tesi nel campo della della categoria Medicina e Chirurgia, in infermieristica e

Evento “Premio Valentina Liboni 2023” 15 dicembre p.v. presso l’Art Hotel di Prato.Evento “Premio Valentina Liboni 2023” 15 dicembre p.v. presso l’Art Hotel di Prato.
Il Presidente e il Comitato Scientifico di IEMIG invitano i Signori Professori, le Autorità, i Soci e gli Amici Sostenitori a partecipare alla cena evento in data 15 dicembre p.v.

Posticipo dell’evento a causa delle condizioni meteorologiche avverse.Posticipo dell’evento a causa delle condizioni meteorologiche avverse.
La Direzione Iemig, in seguito agli eventi meteorologici catastrofici verificatisi nelle ultime 48 ore nella nostra città e considerando i disagi attuali e futuri, ha deciso di posticipare l’evento “Premio
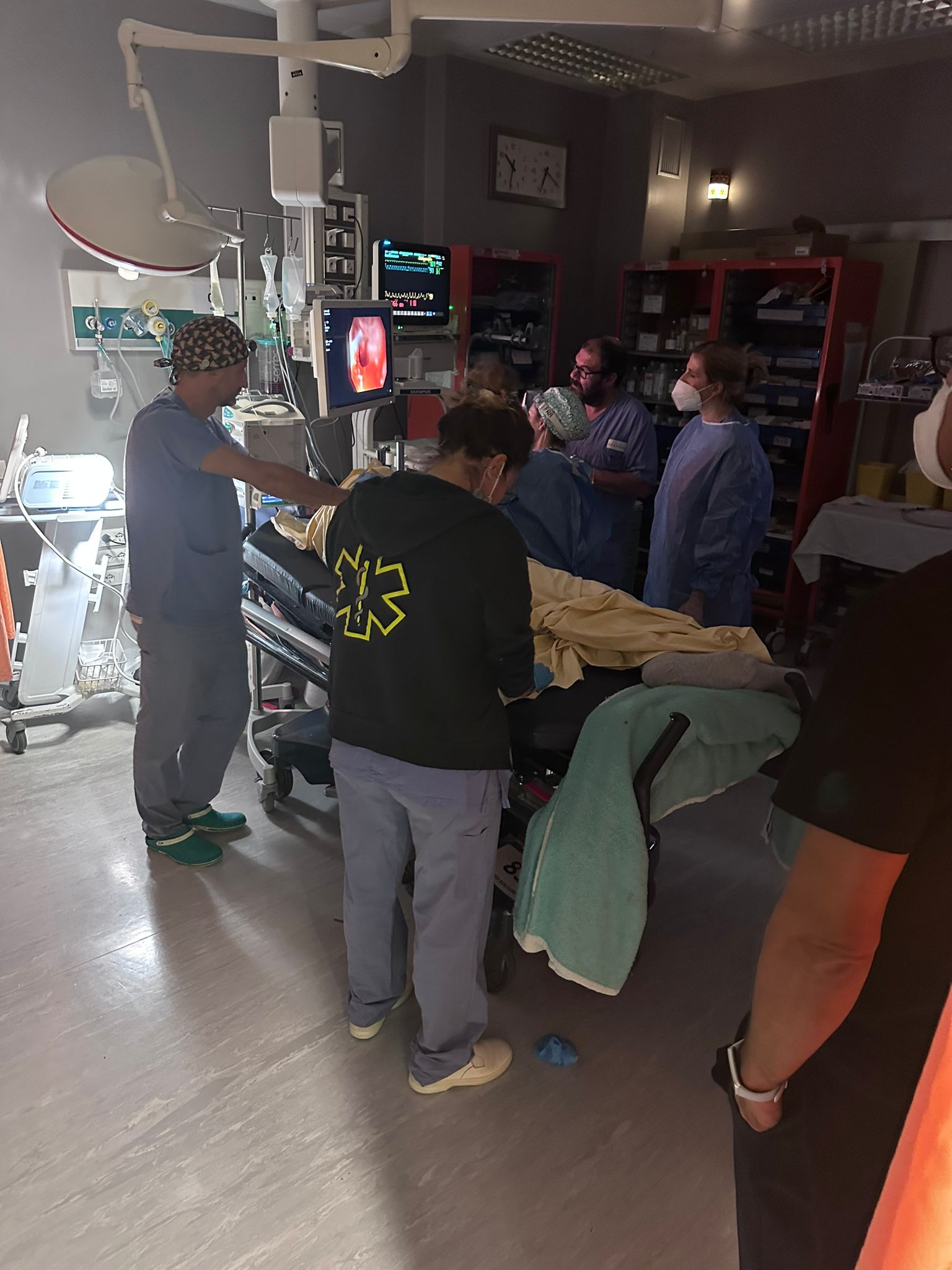
Life in ER- the best medicine “La Vita nell’Unità di Terapia Intensiva: Un Mondo di Sfide e Speranza”Life in ER- the best medicine “La Vita nell’Unità di Terapia Intensiva: Un Mondo di Sfide e Speranza”
La SHOCK ROOM DEL PRONTO SOCCORSO (SALA ROSSA) è un luogo affascinante e impegnativo, dove la vita e la morte si sfidano ogni giorno. I professionisti che lavorano in queste

Premio Valentina Liboni 2023Premio Valentina Liboni 2023
Siamo entusiasti di condividere con te che ci sono ancora posti disponibili per questa occasione unica! L’evento si terrà il l’ 8 Novembre 2023 presso Operà Art & Restaurant –

Decennale di attività del Nuovo Ospedale S. Stefano di PratoDecennale di attività del Nuovo Ospedale S. Stefano di Prato
Il Presidente IEMIG Dr. Alessio Baldini con le Associazioni di Volontariato

A scuola va in scena la lezione di pronto soccorso: medici prof per un giorno. [VIDEO]A scuola va in scena la lezione di pronto soccorso: medici prof per un giorno. [VIDEO]
Succede al Convitto Cicognini con le classi terze della secondaria di primo grado. La prossima settimana nuove lezioni con le prime e le seconde. Massaggio cardiaco con braccia distese e

PREMIO VALENTINA LIBONI 2023PREMIO VALENTINA LIBONI 2023
IEMIG nel 2023 ripresenta il PREMIO VALENTINA LIBONI – il premio sarà riservato alle migliori tesi di laurea in medicina, specializzazione in medicina di urgenza e laurea in scienze infermieristiche,

Traumi addominali chiusiTraumi addominali chiusi
Una lezione sui traumi addominali chiusi a cura della Dott.ssa Stefania Salti e Dott. Andrea Bulli – UO Radiologia, Nuovo Ospedale di Prato Santo Stefano.

Il ruolo del medico e dell’infermiere di PS nella rete di donazione/trapiantoIl ruolo del medico e dell’infermiere di PS nella rete di donazione/trapianto
A cura della Dott.ssa Sara Bagatti, Coordinatrice locale alla donazione di organie tessuti del Nuovo Ospedale Santo Stefano di Prato e dell’Azienda Ospedaliero Universitaria Careggi, nonchè coordinatrice dell’Area Vasta Toscana
IEMIG …..l emergenza si apre alla cittàIEMIG …..l emergenza si apre alla città
Grazie ad AMI ( associazione ONLUS Materno Infantile . Ospedale Santo Stefano – PRATO) – IEMIG ha partecipato alla Giornata della FESTA DELLA MAMMA” , manifestazione tenutasi nei nuovi giardini
Antibiotici in DEA – razionale e peculiaritàAntibiotici in DEA – razionale e peculiarità
Antibiotici in Pronto Soccorso , argomento dibattuto ! linee guida che indirizzano ( con classi di evidenza elevate) la precoce somministrazione degli antibiotici già nelle sale di emergenza e talora
IEMIG – La passione per la Medicina d’UrgenzaIEMIG – La passione per la Medicina d’Urgenza
IEMIG – Italian Emergency Medicine Interest Group – continua con il consueto impegno a diffondere la cultura della medicina d’Urgenza – Il Canale YOUTUBE IEMIG ha raggiunto oltre 900 iscritti
Emergenze OstetricheEmergenze Ostetriche
In Molti Pronto Soccorso le pazienti con patologia ostetrica hanno accesso diretto in Ginecologia: in molti altri contesti è il medico di emergenza che “APPROCCIA” per primo quadri clinici ostetrici.
SERATA EVENTO IEMIG .- TG TOSCANA TVSERATA EVENTO IEMIG .- TG TOSCANA TV
SERATA EVENTO – Presentazione IEMIGSERATA EVENTO – Presentazione IEMIG
23 sett 2021 – Serata eccezionale all ART MUSEUM HOTEL & Restaurant -Tutte le autorità cittadine di Prato con oltre 100 ospiti hanno onorato con la loro presenza la serata
Emergenze pediatricheEmergenze pediatriche
Approccio al paziente pediatrico critico in PS
shock non traumaticoshock non traumatico
La Drssa Rovereto ci illustra sapientemente e in modo esaustivo la tematica dello shock non traumatico. Noi medici di emergenza urgenza sappiamo come molte volte lo shock abbia presentazioni subdole
IEMIG on PressIEMIG on Press
IEMIG inizia a muovere i primi passi proiettandosi all’ esterno delle mura ospedaliere- Il senso di responsabilità degli operatori sanitari verso la comunità e il senso di responsabilità della comunità
La sepsiLa sepsi
Gli anni 2000 sono stati per la sepsi come gli anni 90 per il dolore toracico : nei PS era un fiorire di chest pain unit, protocolli accelerati, mioglobina, troponina,
Gestione delle Vie aereeGestione delle Vie aeree
Ecco un nuovo appuntamento del CANALE IEMIG: gestione delle vie aeree , tematica molto sentita dal medico di emergenza urgenza . Molte volte il contesto ambientale in cui il medico
IEMIG – – RebornIEMIG – – Reborn
Il progetto IEMIG nasce nel 2010 – iniziato con un BLOG e con una sezione che doveva essere una WEB TV- Nonostante l idea originale e anticipatoria , rispetto a

